Leukemia Drugs List: Common Medicines for CML, AML, ALL & CLL
Leukemia is a group of blood cancers that affect the bone marrow and blood-forming tissues, leading to abnormal growth of white blood cells. Treatment depends on the specific type of leukemia, disease stage, genetic mutations, patient age, and overall health.
Modern leukemia treatment includes targeted therapy, chemotherapy, immunotherapy, monoclonal antibodies, stem cell transplantation, and supportive care. Unlike older one-size-fits-all treatment approaches, today’s therapy is increasingly personalized based on molecular testing and treatment response.
This guide explains the most commonly used leukemia medicines for Chronic Myeloid Leukemia (CML), Acute Myeloid Leukemia (AML), Acute Lymphoblastic Leukemia (ALL), and Chronic Lymphocytic Leukemia (CLL), including how these drugs work, when they are used, and important safety considerations.
Understanding Leukemia and Treatment Approaches
Leukemia arises from abnormal production of white blood cells in the bone marrow. The four main types are acute lymphoblastic leukemia (ALL), acute myeloid leukemia (AML), chronic myeloid leukemia (CML), and chronic lymphocytic leukemia (CLL). Treatment goals may include achieving remission, controlling disease progression, managing symptoms, and improving quality of life.
Modern leukemia treatment often combines different drug classes:
- Chemotherapy: Traditional agents that kill rapidly dividing cells.
- Targeted therapy: Drugs that interfere with specific proteins or pathways in cancer cells.
- Immunotherapy: Treatments that help the immune system recognize and attack leukemia cells.
- Supportive care drugs: Medications to manage side effects or complications.
Choice of drugs depends on genetic markers (e.g., Philadelphia chromosome in CML or Ph+ ALL), mutations (e.g., FLT3 or IDH in AML), disease phase, and patient health.
Common Leukemia Drugs by Type
Chronic Myeloid Leukemia (CML) Medications
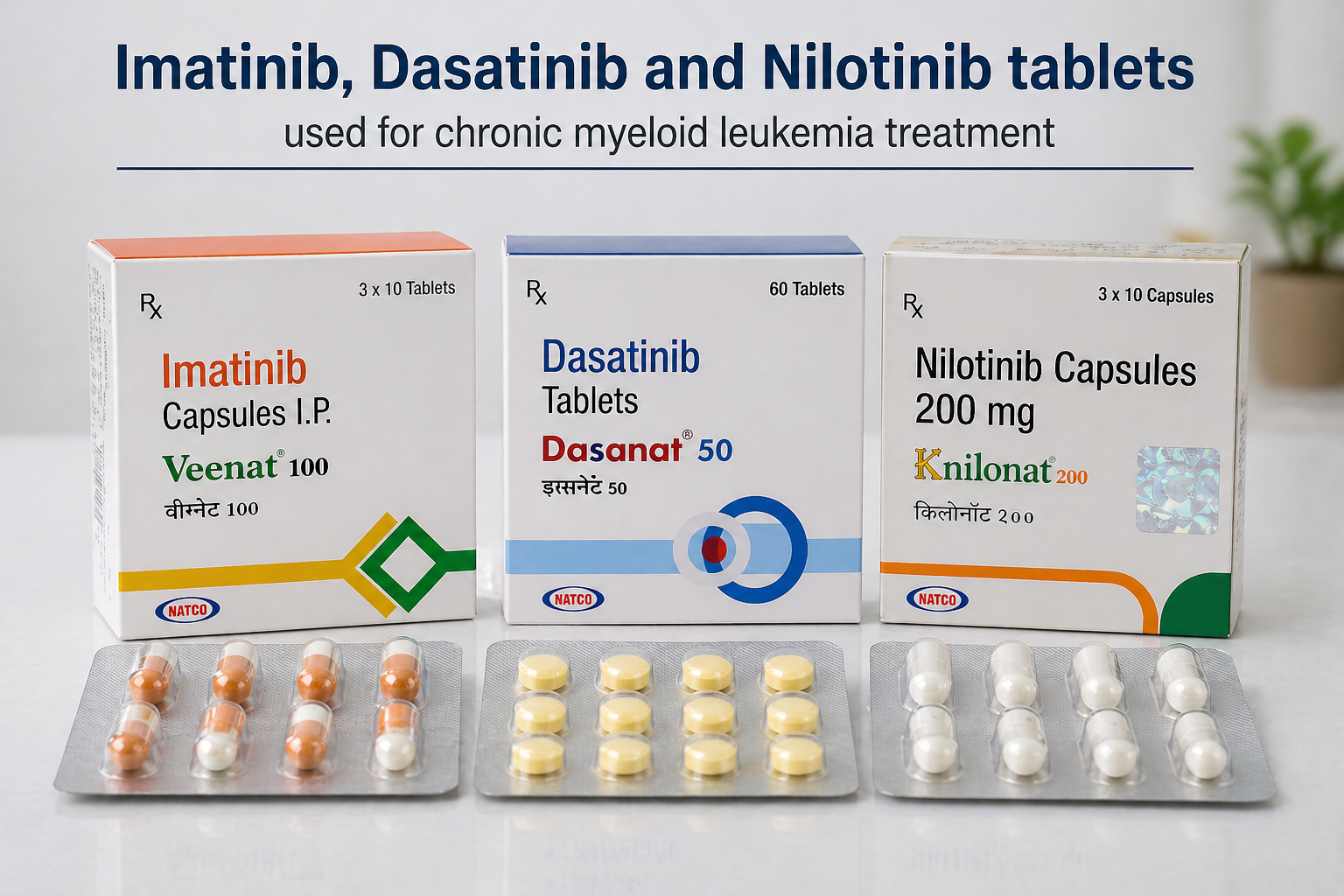
The cornerstone of CML treatment is targeted therapy with tyrosine kinase inhibitors (TKIs) that block the BCR-ABL protein produced by the Philadelphia chromosome.
Common TKIs include:
- Imatinib (Gleevec, Imkeldi)
- Dasatinib (Sprycel)
- Nilotinib (Tasigna, Danziten)
- Bosutinib (Bosulif)
- Ponatinib (Iclusig)
- Asciminib (Scemblix) – an allosteric inhibitor with a different binding mechanism.
These oral medications have dramatically improved outcomes for many patients with chronic-phase CML. In advanced phases, chemotherapy or other approaches may be combined.
Acute Lymphoblastic Leukemia (ALL) Medications
ALL treatment often involves multi-phase chemotherapy regimens, sometimes combined with targeted or immunotherapy agents, especially in Ph+ ALL or relapsed/refractory cases.
Common chemotherapy components include:
- Vincristine
- Daunorubicin or doxorubicin (anthracyclines)
- Cyclophosphamide
- Cytarabine
- Methotrexate
- Asparaginase formulations (e.g., pegaspargase, calaspargase pegol)
- Corticosteroids (prednisone, dexamethasone)
Targeted options for Ph+ ALL may include TKIs such as dasatinib or imatinib. Immunotherapies like blinatumomab (Blincyto), inotuzumab ozogamicin (Besponsa), or CAR-T therapies (e.g., tisagenlecleucel) are used in specific relapsed or high-risk settings.
Acute Myeloid Leukemia (AML) Medications
AML treatment frequently starts with intensive induction chemotherapy (e.g., “7+3” regimen with cytarabine plus an anthracycline). Targeted agents are added based on mutations.
Examples of targeted therapies in AML:
- FLT3 inhibitors: Midostaurin (Rydapt), gilteritinib (Xospata), quizartinib (Vanflyta)
- IDH inhibitors: For IDH1 or IDH2 mutations
- BCL-2 inhibitor: Venetoclax (often combined with azacitidine or low-dose cytarabine for older or unfit patients)
- Other agents: Gemtuzumab ozogamicin (Mylotarg) for CD33-positive AML
Hypomethylating agents like azacitidine or decitabine may be used in lower-intensity regimens.
Chronic Lymphocytic Leukemia (CLL) Medications
CLL treatment has shifted toward targeted therapies rather than traditional chemotherapy for many patients.
Common options include:
- BTK inhibitors: Ibrutinib (Imbruvica), acalabrutinib (Calquence), zanubrutinib (Brukinsa)
- BCL-2 inhibitor: Venetoclax (Venclexta), often combined with obinutuzumab or ibrutinib
- Monoclonal antibodies: Rituximab, obinutuzumab
Chemoimmunotherapy (e.g., fludarabine, cyclophosphamide, rituximab – FCR) may still be appropriate for selected fit patients without certain high-risk features.
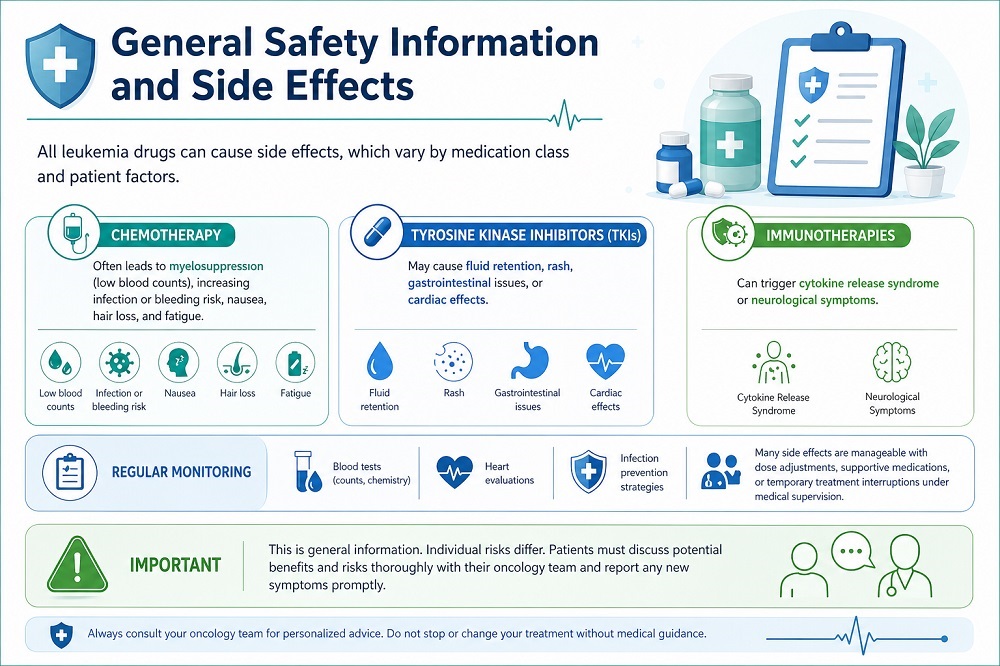
General Safety Information and Side Effects
All leukemia drugs can cause side effects, which vary by medication class and patient factors. Chemotherapy often leads to myelosuppression (low blood counts), increasing infection or bleeding risk, nausea, hair loss, and fatigue. TKIs may cause fluid retention, rash, gastrointestinal issues, or cardiac effects. Immunotherapies can trigger cytokine release syndrome or neurological symptoms.
Regular monitoring with blood tests, heart evaluations, and infection prevention strategies is standard. Many side effects are manageable with dose adjustments, supportive medications, or temporary treatment interruptions under medical supervision.
Important: This is general information. Individual risks differ. Patients must discuss potential benefits and risks thoroughly with their oncology team and report any new symptoms promptly.
Factors Influencing Leukemia Drug Selection
Oncologists consider multiple factors when building a treatment plan:
- Leukemia subtype and genetic profile (e.g., Philadelphia chromosome, FLT3, TP53 mutations)
- Disease stage or risk category
- Patient age, overall health, and comorbidities
- Prior treatments and response
- Goals of care (curative intent vs. disease control)
Treatment is dynamic—patients may switch drugs due to resistance, intolerance, or disease progression. Stem cell transplantation remains an important option for eligible patients with high-risk or relapsed disease.
FAQs About Leukemia Drugs

What are the main drugs used to treat leukemia?
Leukemia treatment uses chemotherapy (e.g., cytarabine, vincristine, anthracyclines), targeted therapies (tyrosine kinase inhibitors like imatinib or dasatinib for CML/Ph+ ALL, BTK inhibitors for CLL), and immunotherapies (blinatumomab, CAR-T cells). The specific combination depends on the leukemia type.
What are the most common targeted therapies for CML?
Tyrosine kinase inhibitors (TKIs) are the primary treatment for CML. Common options include imatinib, dasatinib, nilotinib, bosutinib, ponatinib, and asciminib. These oral drugs target the BCR-ABL protein.
Which drugs are used in acute lymphoblastic leukemia (ALL)?
ALL regimens often include multi-agent chemotherapy with vincristine, corticosteroids, anthracyclines, asparaginase, methotrexate, and cytarabine. Targeted TKIs are added for Ph+ ALL, and immunotherapies like blinatumomab may be used in relapsed cases.
Are there targeted drugs for acute myeloid leukemia (AML)?
Yes. Depending on mutations, FLT3 inhibitors (midostaurin, gilteritinib), IDH inhibitors, venetoclax (BCL-2 inhibitor), and gemtuzumab ozogamicin may be combined with chemotherapy or used in lower-intensity regimens.
How do tyrosine kinase inhibitors work in leukemia?
TKIs block specific enzymes (kinases) that drive leukemia cell growth, such as BCR-ABL in CML and Ph+ ALL. This targeted approach can lead to deep responses with generally fewer broad effects than traditional chemotherapy.
Can leukemia be treated with oral medications only?
Many patients with CML or CLL can be managed primarily with oral targeted therapies. However, acute leukemias (ALL and AML) usually require initial intravenous chemotherapy, sometimes followed by oral maintenance or targeted agents.
What are common side effects of leukemia drugs?
Side effects vary widely. Chemotherapy often causes low blood counts, nausea, and fatigue. TKIs may cause rash, diarrhea, fluid retention, or muscle pain. Immunotherapies can trigger immune-related reactions. Close monitoring helps manage these effects.
Is there a single best drug for all types of leukemia?
No. Each leukemia type and patient requires a tailored approach. What works well for CML (e.g., TKIs) is not suitable as standalone therapy for most AML or ALL cases.
Are generic versions available for leukemia medications?
Yes. Generics exist for several older TKIs (e.g., imatinib, dasatinib) and many chemotherapy agents, which can improve affordability. Newer targeted drugs may still be available only as brand-name products.
How long do patients typically take leukemia drugs?
Duration varies. CML patients often continue TKIs long-term or indefinitely. ALL and AML treatment includes intensive phases followed by consolidation or maintenance, sometimes lasting years. Decisions are guided by response monitoring.
Can new leukemia drugs be used in combination?
Yes. Many modern regimens combine chemotherapy with targeted agents or immunotherapy to improve outcomes while trying to reduce toxicity. Clinical guidelines evolve as new data emerge.
What should patients know before starting leukemia treatment?
Discuss the specific drugs planned, expected side effects, monitoring schedule, fertility preservation options (if relevant), and financial/support resources with your care team. Adherence and open communication are essential.
Conclusion
A comprehensive **leukemia drugs list** reflects the significant advances in oncology over recent decades. From traditional chemotherapy to highly targeted tyrosine kinase inhibitors and innovative immunotherapies, treatment options continue to expand, allowing more personalized approaches for CML, ALL, AML, CLL, and other subtypes.
While these medications have improved survival and quality of life for many patients, successful outcomes depend on accurate diagnosis, expert medical management, regular monitoring, and individualized care plans. No single drug or list applies universally.
If you or a loved one has been diagnosed with leukemia or are seeking more information about treatment options, consult your healthcare provider promptly. Hematology-oncology specialists, leukemia support organizations, and multidisciplinary teams can provide the most appropriate guidance and support tailored to your needs.
Disclaimer: This article is educational and based on general information about commonly used medications in leukemia. It does not replace professional medical advice, diagnosis, or treatment. Drug approvals, indications, and practices change over time. Always rely on your physician’s recommendations and the latest clinical guidelines.
